Community-Facility Integration: Accelerated TB Case Detection, Community Rights, and Gender (CRG) Advocacy
Bungoma County, Kenya | January-November 2024

Official Document | AIGHAP Impact Brief Repository
Background
The African Initiative for Global Health, Advocacy, and Policy (AIGHAP) implemented the TB CRG Wave 11 grant under the auspices of Stop TB Partnerships Kenya between January and November 2024. AIGHAP sought to increase participation, accountability, non-discrimination, empowerment, linkage, and sustainability among vulnerable and marginalized populations affected by TB in Bungoma, Kenya, through PANELS for TB in Kenya (PANELS K). The program deployed 20 TB champions and one coordinator across 10 health facilities in six subcounties, and assessed performance pre-implementation (2023) and during implementation (2024, January-September).
Between 2023 and 2024, community-facility case-finding activities screened 145,575 individuals, resulting in 652 confirmed TB diagnoses and 652 treatment initiations. Community TB champions enabled 306 diagnoses, representing 46.9% of all detected cases. The program recorded a diagnostic yield of 10.3%, number needed to screen (NNS) of 372.3, and number needed to test (NNT) of 9.7.
Community outreach reached transport corridor workers, substance users, migrants, prisoners, and other underserved populations. Geographic and facility analyses identified key diagnostic hotspots, and the overall detection rate reached 447.9 TB cases per 100,000 screened. Findings show that integrating trained TB champions into community health systems strengthens early detection, community-facility linkage, and TB notification among vulnerable populations.
Implementation
Across 10 integrated facilities, TB champions were institutionally embedded as supervised community-facility actors. This integration improved symptom screening, referral completion, and treatment linkage by combining facility workflow discipline with hotspot intelligence.
Diagnostic cascade tracking demonstrated strong continuity from screening through treatment initiation. No diagnosed client was lost before treatment start, signaling robust coordination between outreach, triage, and clinical teams.
Champion contribution scaled across implementation, increasing from 23.7% in January to 47.7% in April and sustaining 46.9% in May. This trend indicates progressive normalization of champion-led diagnostic support inside routine operations.
The rights and vulnerability lens remained central to delivery. Men in hotspot zones faced delayed care due to alcohol dependency and unstable income, while women and girls reported stigma, GBV-linked constraints, food insecurity, and psychosocial pressure affecting adherence.
Adolescents and youth encountered school-based stigma and continuity barriers, while substance-dependent populations faced interruption risks associated with homelessness and food insecurity. Support groups functioned as practical adherence and stigma-reduction platforms.
Despite delayed operational clearance and strike disruption, a $50,000 grant produced 306 champion-enabled diagnoses (about $163 per diagnosis), indicating strong value-for-investment under constrained implementation conditions.
CFI Model (Scaled)
CFI (TM) - Community-Facility Integration Model
Structured Diagnostic Acceleration Framework: Embeds trained community actors into facility diagnostic workflows; accelerates case detection; preserves cascade integrity; institutionalizes integration.
- Facility Embedding - Formal assignment and supervision
- Hotspot Intelligence - Mapped high-burden deployment
- Governance Supervision - Routine performance cadence
- Data-Embedded Reporting - Integrated reporting channels

Program Performance
Facility and Program Outputs
| Total workload | 184,179 |
| Individuals screened | 145,575 |
| Presumptive TB cases | 4,534 |
| Individuals evaluated | 2,845 |
| TB cases diagnosed | 652 |
| Treatment initiations | 652 |
| Champion-enabled diagnoses | 306 |
| Champion contribution (%) | 46.9 |
| Champion productivity (cases/champion) | 14.6 |
Community Outreach Cascade and Key Metrics
| Screened (cascade sample) | 644 |
| CXR triage | 436 |
| Investigated | 266 |
| Diagnosed | 26 |
| Initiated treatment | 26 |
| Diagnostic yield (%) | 10.3 |
| Number needed to screen (NNS) | 372.3 |
| Number needed to test (NNT) | 9.7 |
| Bacteriological confirmation (%) | 44.9 |
| Detection rate (per 100,000 screened) | 447.9 |
Framework Alignment
- WHO End TB Strategy - Pillar 1
- Global Fund Strategic Objective 2
- Sustainable Development Goals - SDG 3.3
Key Program Outputs
- 652 Facility TB Diagnoses
- 306 Champion-Enabled Diagnoses
- 652 Treatment Initiations
- 46.9% Champion Contribution
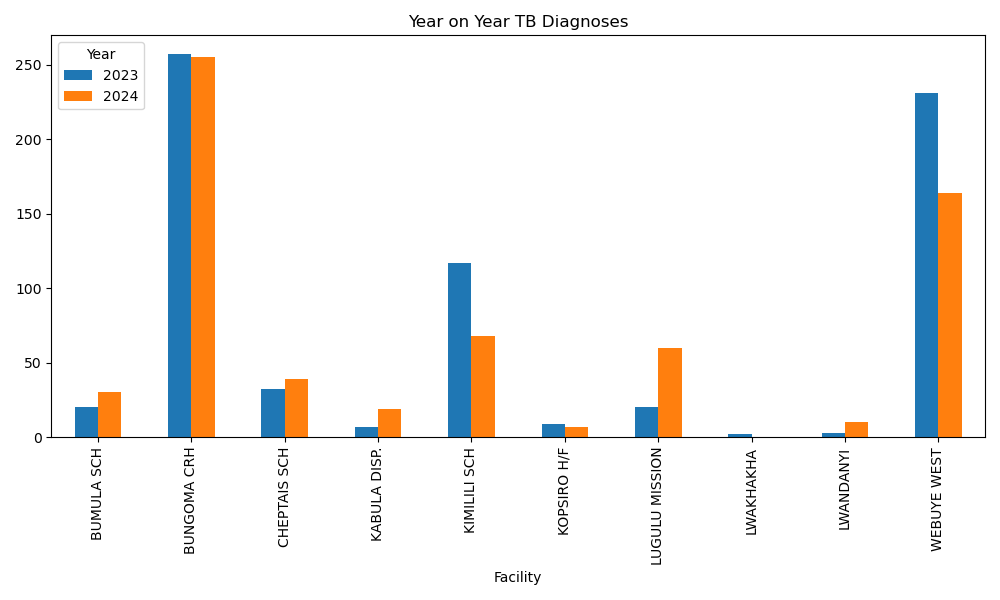
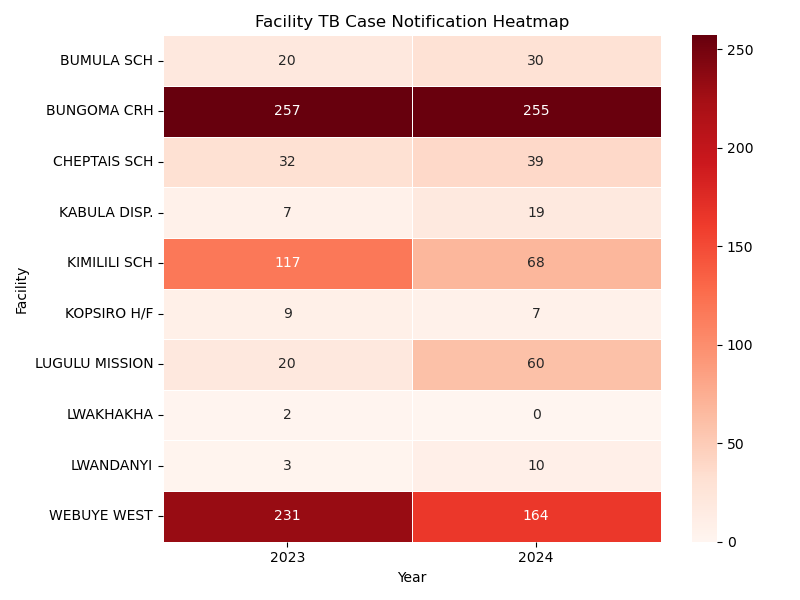
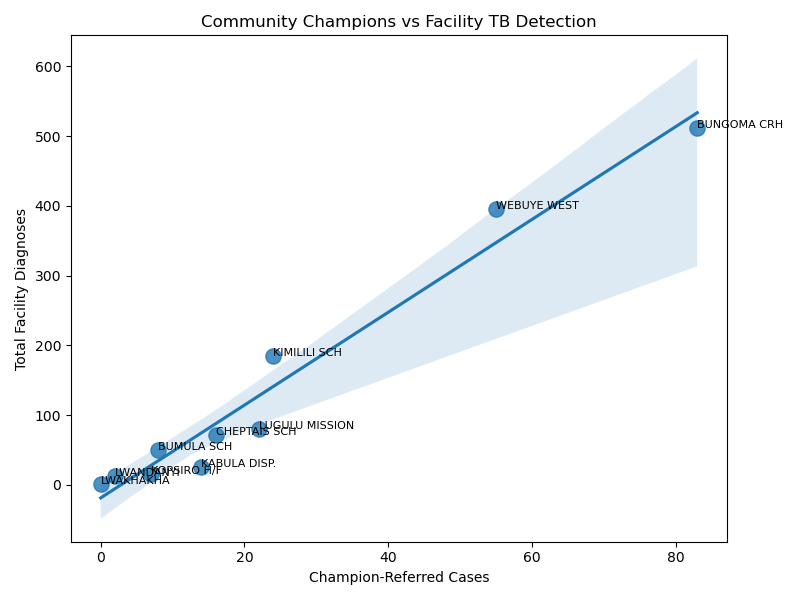
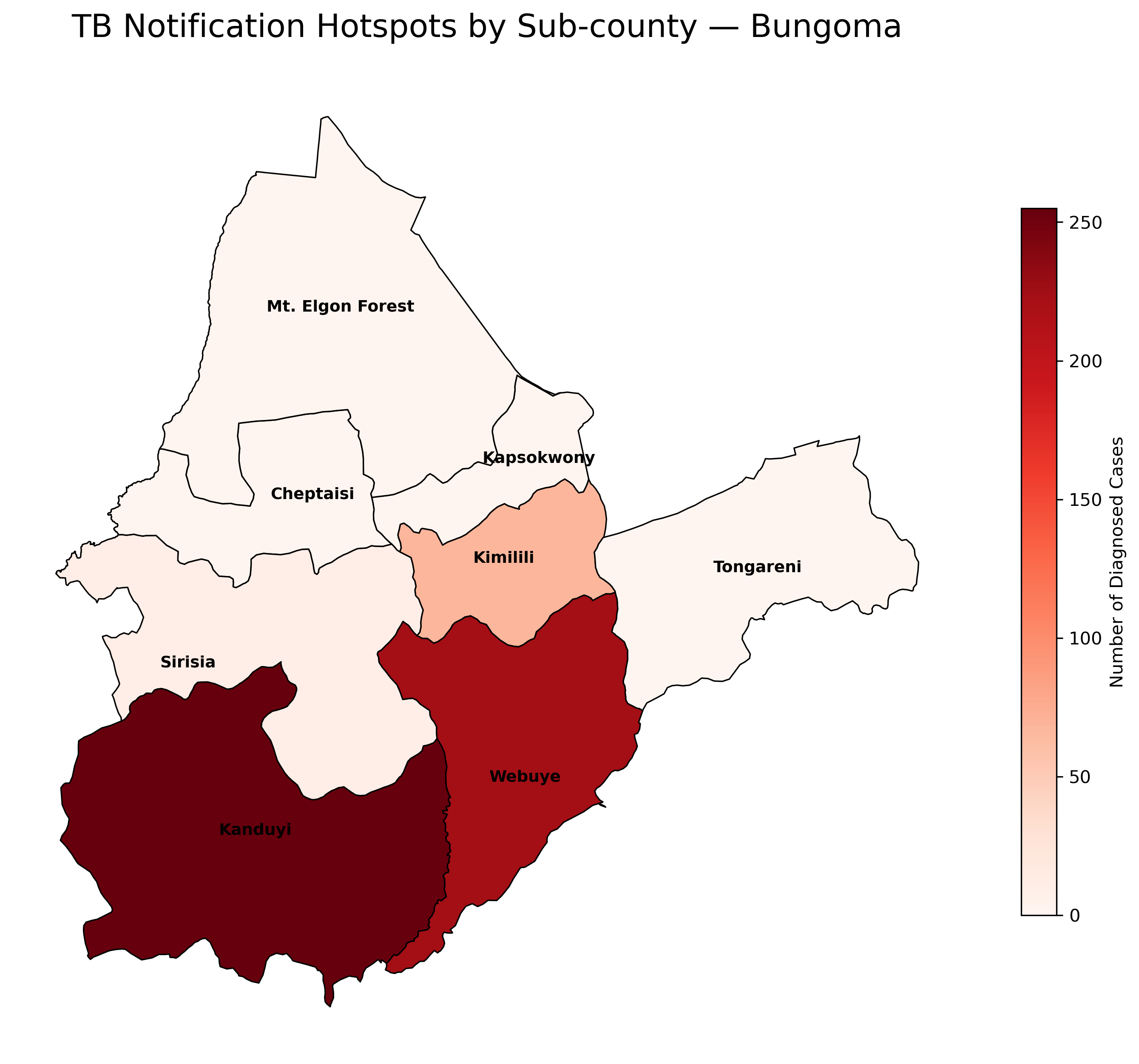
Figure: CFI implementation evidence visuals (facility trend, heatmap, champion contribution elasticity, and hotspot map).
Key Vulnerable Populations (KVPs) Reached
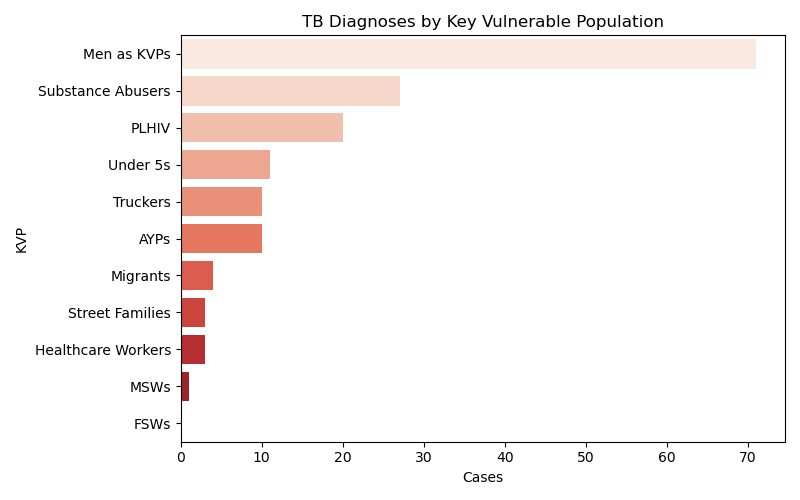
Community Rights, Gender, and Engagement Highlights
Community Rights and Gender Integration
- PANELS framework implemented across Wave 11 delivery.
- Champions acted as trusted community-facility intermediaries.
- Champion-enabled referrals delivered 306 diagnoses (46.9%).
Gender Equity Analysis
- Gender-responsive design integrated throughout outreach.
- Both male and female champions trained and deployed.
- Champion-detected cases included both male and female patients.
Community Engagement Indicators
- TB champions trained.
- Outreach and screening events conducted.
- Support groups and awareness activities implemented.
- Referral linkage between communities and facilities strengthened.
Community Engagement Impact
- Improved TB awareness in target communities.
- Enhanced psychosocial support for TB patients.
- Reduced stigma and discrimination barriers.
- Improved adherence and community-facility linkage.
Social Determinants Identified
- Food insecurity among TB patients.
- Stigma and discrimination affecting care seeking.
- Delayed diagnosis after initial private facility care.
- Substance use and economic vulnerability affecting adherence.
Programmatic Lessons
- Community TB champions improve case detection among marginalized populations.
- Support groups provide safe psychosocial spaces.
- Community outreach strengthens hotspot-to-facility linkage.
- Community-facility collaboration improves early detection and initiation.
Policy Implications
- Increase early TB case detection through community-led approaches.
- Reduce stigma and discrimination in TB care.
- Strengthen treatment adherence through community support.
- Improve engagement with vulnerable and marginalized populations.
Scalability
- Integrating trained TB champions strengthens early TB detection.
- Improves linkage between vulnerable communities and facilities.
- Supports expansion to additional high-burden settings.

Acknowledgements
We gratefully acknowledge the Stop TB Partnership's TB REACH initiative for supporting this research/program through a Wave 11 grant. The project was designed to increase Participation, Accountability, Non-discrimination, Empowerment, Linkage and Sustainability among vulnerable and marginalized populations affected by TB in Bungoma Kenya, and was supported by funding from Global Affairs Canada. Stop TB Partnership is hosted by UNOPS.
Language note: This brief applies people-centered, non-stigmatizing language in line with Stop TB Partnership guidance.











Brief Workflow
Preview and download workflow for this brief is available in Impact > Reports & Evidence.